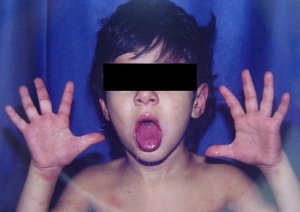
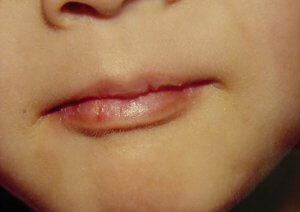
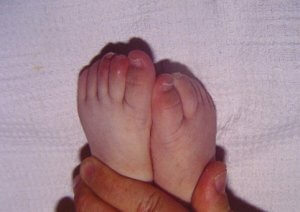
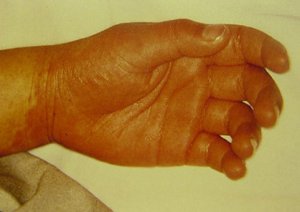
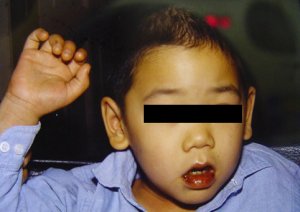
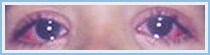
Taken from: Vainstein E., Baleani S. Enfermedad de Kawasaki casos incompletos o atípicos. Estrategia diagnóstica. Revista del Hospital de Niños (B. Aires) 2007; 49(222): 93-98.
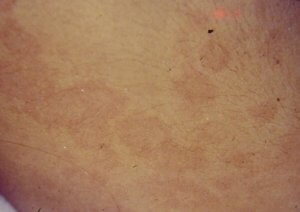
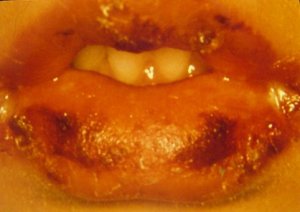
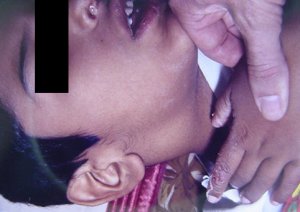
1 Children ≤6 months old, after ≥7 days of unexplained fever: must undergo lab tests and if there is evidence of systemic inflammation an echocardiogram must be done, even in the absence of clinical criteria. 2 See Diagnosis criteria. Characteristics that suggest another disease: exudative conjunctivitis, exudative pharyngitis, mild intraoral lesions, bullous exanthems or generalized adenopathy. Consider alternative diagnoses. 3 Laboratory criteria: albumin ≤3 g/dl, anemic for such an early age, increased alanine aminotransferase, platelet recount ≥450.000/mm3 after 7 days, white blood cells recount ≥15.000/mm3 and urine with ≥10 white blood cell/field. 4 Can be treated before the echocardiogram. 5 Echocardiogram: consider as positive the presence of perivascular refractivity, reduced left ventricular function, mitral regurgitation, pericardial effusion, lumen diameter of coronary arteries >3 mm in <5-year-olds, and >4 mm in >5-year-olds; if the diameter of a segment measures ≥1,5 times the adjacent segment or in relation to the aorta, or if there are irregularities in the coronary lumen. The echocardiogram must be done by a trained professional. 6 Pathological ECG: arrhythmia, tachycardia, prolonged PR interval, low QRS voltage, changes in ST-T waves, abnormal Q waves, repolarization disorders. 7 If the echocardiogram or the ECG are positive, treatment must be administered within 10 days since the fever started, and after 10 days, patients with lab (C reactive protein, erythrocyte sedimentation) and clinical signs that indicate inflammation. 8 Typical desquamation starts under the nail bed of fingers and soon after, toes. CRP: C reactive protein. ESR: erythrocyte sedimentation rate. Echo: echocardiogram. KD: Kawasaki disease.